The other day while I was suturing a patient’s laceration in the ED, he began to ask me some great questions about the aftercare for his injury. While I had a standard set of “canned” answers to give, it made me realize that I wasn’t quite so sure about the legitimacy of my responses. Most of it was based on things my mentors had taught me, things I believed from my own anecdotal experiences in patient follow up, and improvisation. But what data did I really have to support what I said? What evidence do we have as a community?
I’ve decided to frame this blog post as the top questions that I feel patients ask us regarding what to do and what to expect with their wound in the first week or so (the period before the sutures come out, and sometimes immediately following), with links to some recent evidence-based publications. Do any of these questions sound familiar to you?
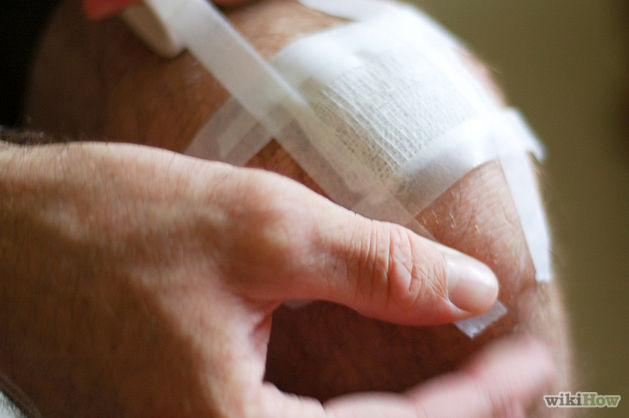 Example of dressing a laceration after repair. Image courtesy of WikiHow, under Creative Commons Liscence (http://creativecommons.org/licenses/by-nc-sa/3.0/).
Example of dressing a laceration after repair. Image courtesy of WikiHow, under Creative Commons Liscence (http://creativecommons.org/licenses/by-nc-sa/3.0/).Patient: “When do I take this dressing off? Do I need to replace it with a new one?”
In my ED, it’s standard practice for a technician to come in and “dress” the wound after it’s been repaired with sutures. What we will typically do is smear antibiotic ointment over the wound, then tape or wrap a dry dressing in place over it. And the patient inevitably (and appropriately) wants to know–how long should it stay there?
You (Short version): Take it off tomorrow. Don’t replace it.
The argument for leaving a dry, absorbent, non-adherent dressing in place is that such a dressing can absorb exudate from the wound, which in turn will keep it dry and clean. Also, the dressing may act as a barrier which prevents bacterial infection from the external environment. The counterargument is that for a very exudative wound, the dressing may saturate and create a moist environment around the wound which can macerate the surrounding tissue or increase bacterial colonization, which is then trapped inside by the overlying dressing. Furthermore, it is harder for a patient to keep tabs on a wound that is covered.
No recent studies in the Emergency Medicine literature that I could find have addressed this question. A Cochrane Review by Toon, et al published in late 2013 asked this question in post-op patients with surgical site incisions. Not quite our population to be sure, but it’s the closest thing out there. They set out to evaluate the risk/benefits of removing a surgical site dressing within 48 hrs without replacement vs leaving the dressing in place with periodic changes until the wound heals. Their review included 3 trials with 280 pts undergoing elective surgery. They found that early dressing removal had no detrimental effect on outcomes. But, the 3 individual studies, though RCTs, were each small, at high risk of bias, and the confidence intervals around the point estimates were quite wide.
Practically speaking, replacing dressings is a hassle for the patient. It makes it harder to identify potential problems with the wound. If it seems like there is no difference in outcomes when you remove the dressing compared with constantly replacing it, why bother?
Patient: “Is it okay to shower/bathe?”
You: Yes, for god’s sake!
If you want your girlfriend/husband/that person you are scheduled for a second date with that you met online to come within 10 feet of you, I suggest that you keep clean. But seriously–this is a very common question patients pose after lac repairs. In my experience, experienced doctors are very good at making up answers to this question with a great deal of confidence. But, personally I had never come across any strong data to guide what we tell patients in these situations. Several of the same authors also reviewed this subject in a Cochrane Library review in 2013 (Toon CD, et al). Again, they looked at this question in the care of patients with post-operative wounds. It’s a given that the sterile post-op wound is quite different than the repaired traumatic laceration, but there may not be any more suitable studies out there to address the question. They examined a study of patients undergoing minor skin excision surgery in the primary care setting. They compared early post-operative bathing (<12 hrs) to delayed bathing (>48 hrs) and found no statistically significant difference in surgical site infections. This said, with only 857 total patients and a low rate of baseline surgical site infection, the Confidence Intervals were way too wide to be certain whether a true difference may exist.
I would always invoke the rules of common sense: intense scrubbing/wiping with a sponge/towel/rag are certain to increase dehiscence risk. With adhesive tapes or glues, the risk of loosening and dehiscence is certainly greater and in general, these wounds should just be kept dry as long and as much as possible. In this situation, a shower with a shorter exposure to water may be preferable to a long bath. But perhaps the best argument for removing a dressing early and cleaning the wound is that it forces the patient to look at the wound early and regularly, so they will be more apt to identify a wound infection earlier.
Patient: “I’ve heard Vitamin E lotion will help reduce scar formation? Should I put this on my wound?”
Have you ever had a patient ask you this? It seems to come up commonly among patients I see.
 Commercially available Vitamin E creams and lotions are widely touted as beneficial to wound healing. But is that the case for traumatic lacerations?
Commercially available Vitamin E creams and lotions are widely touted as beneficial to wound healing. But is that the case for traumatic lacerations?Vitamin E was discovered in 1922 by researchers at the University of California who suggested it could be of benefit in wound healing and scar repair. As an anti-oxidant (buzzword alert), it stabilizes cell membranes, reducing the chemicals released by inflammatory cells. Thus, apply it to the injured area for a prettier wound.
Sounds great, theoretically, but this has not borne out well in studies. In fact, some studies suggest a potential detrimental effect in that patients can develop hypersensitivity reactions, urticaria, dermatitis, even erythema multiforme! In fact, in one study there was a suggestion that cosmetic outcome with Vitamin E lotion in the population at large may actually be worse, in part because of these risks. A great reference for this was published in 2006 by Khoosal and Goldman. Certainly, more research and better, bigger studies are needed before this can be made a standard recommendation. If a patient insists, make sure they use it on intact skin after the initial wound healing has occurred and that they have proven tolerance to Vitamin E in the past.
That’s enough weak evidence for one week. Are there any questions you’ve gotten from patients regarding post laceration repair wound care that you’d like me to address? Also, just for fun, what are some of the stranger and more outlandish questions you’ve been asked? Post your responses here!

