Case Study
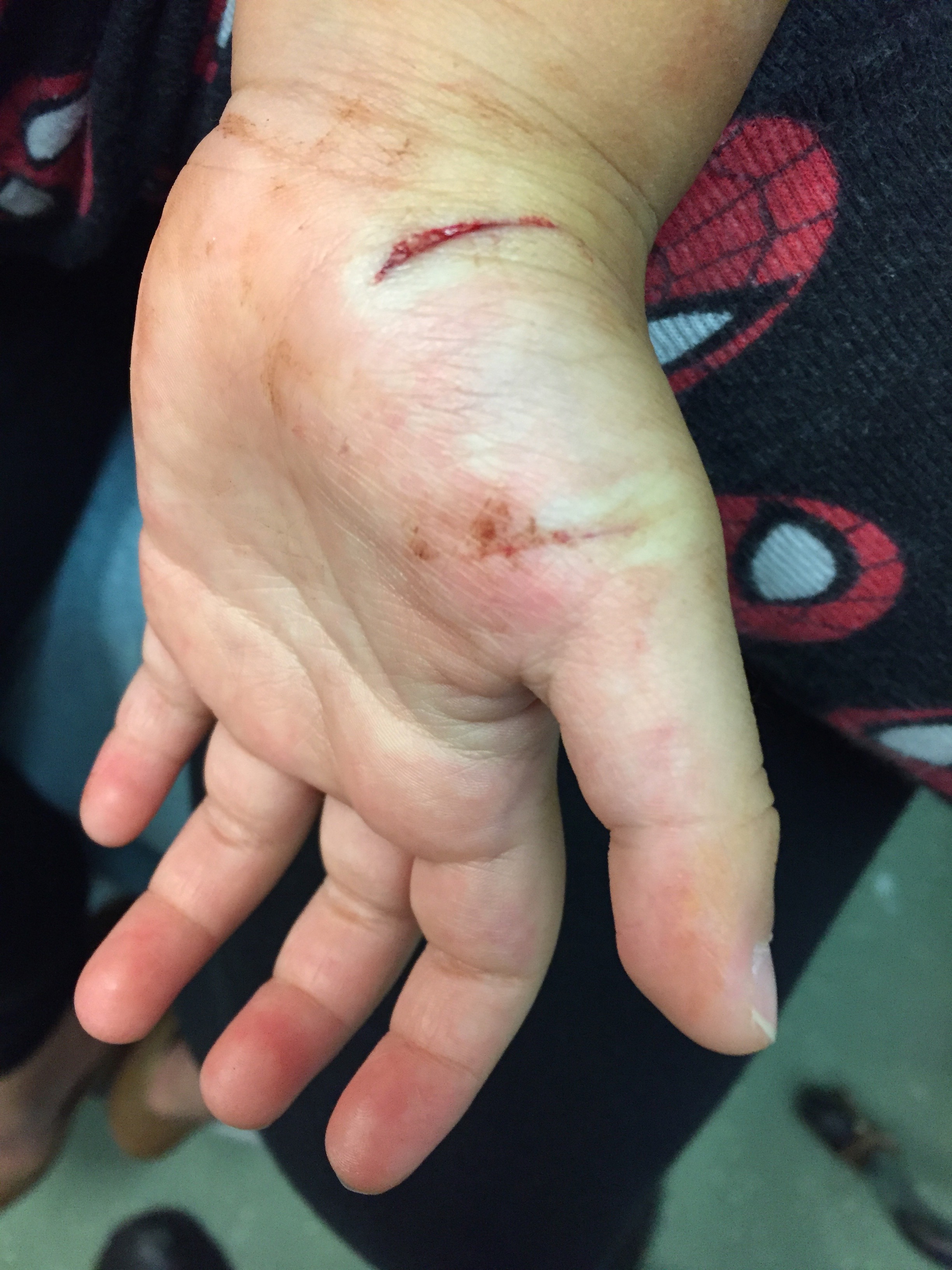
A young, otherwise healthy male dog walker presents within hours of a dog bite laceration to his hand, just distal to the crease of his wrist. Perfect cosmesis is not an expectation, but without some type of closure, he is going to be left with a pretty noticeable scar—a few simple interrupted or vertical mattress sutures could really help this situation and still leave plenty of openings for the wound to drain.
One of your colleagues in a surgical residency mentioned to you that with high-risk surgical wounds, they sometimes close “loosely” with sutures or staples, in order to allow the wound to drain and prevent abscess formation.
You wonder if this “loose closure” strategy could be appropriate for this patient, and what evidence exists to support it.
The Clinical Question
What exactly is “loose” closure? Is there a role for loose closure in taking care of traumatic lacerations?
Introduction
From time to time, I will hear physicians refer to “loose closure” as a strategy for dealing with selected high risk wounds. But is this a real thing? What is the origin of this strategy? And are there any good studies to back it up in emergency wound care?
Why might you use loose closure in Emergency Medicine?
There are several candidate wounds that could potentially benefit from a loose closure strategy, in efforts to mitigate infection risk:
- Highly contaminated wounds (such as dog bites, and other grossly soiled wounds)
- Delayed presentation (wounds treated outside of the golden period are traditionally considered higher risk)
- Patients with risk factors for wound infection per Quinn’s 2014 study (DM, wound >5cm, lower extremity)
- AND wounds in a body area (as judged by the patient) where better cosmesis may be desired, but isn’t critically important
The origin of loose closure
I tackled this subject with Dr. Julie Vieth (@julieTVieth), a practicing Emergency Physician in New York. We did a deep dive in to the literature, and here is what we found:
The first real description of loose closure we found in our literature search was this 1993 study. During a 9-year period, 183 consecutive patients underwent total colectomy and the endorectal ileal pull-through procedure (ERIPT) for ulcerative colitis (UC), familial polyposis, or Hirschsprung’s disease. Their control group (“1A”) had primary closure of their abdominal wounds, while receiving perioperative antibiotics. In contrast, their study group (“2A”) had the same closure PLUS an additional intervention: the wounds were probed daily in four to six sites for the first five postoperative days with a Q-tip moistened with 2% aqueous mercurachrome solution. They spaced staples 1.5 cm apart, and probed between them. They found an astoundingly lower wound infection rate for the group 2A patients (4.3%) versus the group 1A patients (24.4%) [P < 0.0001, ANOVA].
While they didn’t term their probing specifically as “loose closure,” this hints at the origin of the terminology. They took a bunch of pretty sick, immunosuppressed patients getting bowel surgery and described actively and routinely probing the abdominal wounds in between staples, effectively “loosening” the closure.
Is this surgical concept generalizable to EM?
To answer this question, we combed through the medical literature in search of any shred of evidence that loose closure was a real thing that had been trialed within emergency departments. (search terms: loose closure; loose closure AND emergency medicine; loose closure AND laceration; loose closure AND traumatic laceration; loose closure AND trauma).
The answer was disappointing: no studies exist in the Emergency Medicine literature (not even low quality ones).
We did, however, find a few studies in the modern surgical literature that are possibly generalizable.
A 2007 study compared loose approximation of skin wounds in patients with perforated appendicitis, versus what they refer to as “perfect cosmetic closure.” In this study, the term “loose closure” was used, but notably this was actually the control group, while “cosmetic” closure with subcuticular sutures was the intervention.
This was not an awesome study, for several reasons:
- No mention of randomization
- 100 patients in each group, no mention of power calculation
- Also, in this study they assume that patients who receive a closure “for better cosmetic results” with 4-0 nylon running subcuticular sutures were happier with their cosmetic outcome. They did not ask the question, survey the patients, or record this as a secondary outcome. It is possible that patients would be happy with the cosmetic result with either closure method.
A second study, from 2013, explores the use of loose closure in an even riskier setting.
In this small study, early scrotal approximation after incision and drainage of Fournier’s gangrene was performed. The authors used a type of loose closure that they termed a “modified U-stitch,” which involved placing a Penrose drain within the closure to facilitate drainage. They found that their U-stitch patients required less hospitalization then patients managed with their usual technique of split thickness skin grafting. Because their study was observational, it was mostly a test of concept.
My take on this:
- While it doesn’t hold up as definitive evidence for obvious reasons, as a proof of concept this is nothing short of amazing. Primary closure of necrotizing fasciitis!!! That takes…well, you know what it takes.
- Not much in terms of study methodology (retrospective, small number of patients, p values don’t meet significance for their endpoint which wasn’t even clearly stated) but still...wow.
- Just the fact that it worked at all, for even one patient, is amazing.
Finally, we examined a third interesting study from 2014. In this study, the authors compared the prevalence of surgical site infection following stoma site closure using 4 different surgical techniques. They performed a retrospective review of all adult patients undergoing stoma reversal, comparing techniques of: primary closure (PC), secondary closure (SC), “loose PC” (LPC), and circular closure (CC). They found that surgical site infection rate was lowest for stomas that were closed using the circular closure method.
My take:
- Stoma closure is obviously not the same thing as closure of a traumatic laceration, but may be a reasonable surrogate–both probably fall in to the contaminated (Class III) wound category.
- This study did show a benefit of loose closure (closing the fascia, then loose approximation of the skin with sutures or staples and packing between the closure points with gauze wicks) over standard closure (fascial closure then skin closure with staples). Surgical site infection rates were highest for PC (43%, mirroring the surgical dogma mentioned before), and only 15% for LPC, which was similar to closure by secondary intention (16%).
- What technically won in this battle royale of techniques was “circular closure” with a purse string and placement of a drain in the middle (6%). In my opinion, also a variation on a theme of loose closure.
If any study out there supports loose closure, that may be the one.
Closing Thoughts & Summary:
“Loose closure” is not a term used to classify wound closure in the EM literature, and though explored in some small surgical studies it’s not clearly defined. As such, it’s ultimately a form of primary closure. Thus we shouldn’t be acting surprised when a wound becomes infected when it was “closed loosely” to “let the infection out.”
- In the ED, our decision is generally pretty binary: closure by primary intention vs by secondary intention. Since most of us can’t guarantee follow up, delayed primary closure is not an option (and a totally separate discussion).
- Keep the decision simple. We just don’t have the evidence to back an approach with different gradations of closure (yet—and we may never have it). For Emergency Medicine purposes, closure is closure is closure.
- We shouldn’t be reassuring ourselves or the patients that loose closure is a better way. If you are going to close, do it in such a way that you and the patient are truly satisfied with the cosmetic outcome achieved.
Case Resolution:
You inform your surgical colleague that the loose closure strategy hasn’t been studied nor proven effective in the Emergency Medicine setting.
You describe to the patient that your general practice in the emergency department is to leave dog bite wounds open in areas that are not highly cosmetic, such as the hand, due to associated infection risk. (The conversation may be different if the wound was on the patient’s face.) He agrees. You properly anesthetize the wound, irrigate it, dress the wound, and prescribe prophylactic antibiotics (also a weak recommendation…a subject for another time!)
Want to hear more? This blog post was based on a discussion between myself and Dr. Julie Vieth (@julieTVieth), a practicing Emergency Physician in New York, which has been posted for your listening pleasure by the good folks at EM:RAP.

