Case Discussion
A few months ago I saw an interesting case of a young man with a small but deep avulsion wound to his dominant hand. He worked as a chef, but as luck would have it his injury occurred while cooking off-duty.
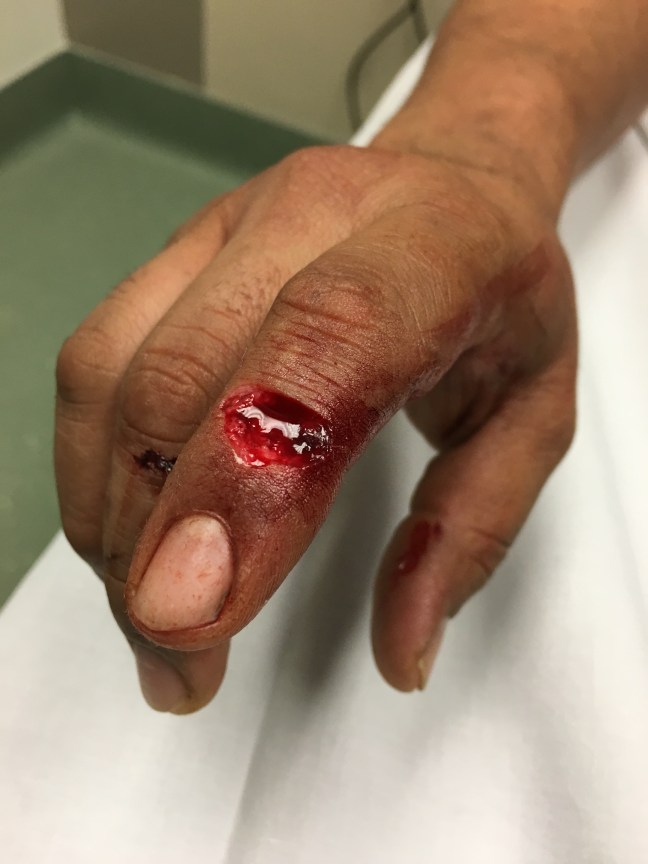
As pictured, his wound involved the extensor surface of his second finger. A slipped knife created a deep pit in the soft tissue of his finger overlying the distal interphalangeal joint crease. Incredibly, no nerve, tendon, or vascular structures were involved.
Still–the wound was deep and disfiguring. I felt something needed to be done.
Unfortunately, the nature of many distal finger injuries is such that when the skin is avulsed, there is rarely enough mobile adjacent soft tissue available to advance and cover the wound. Further, aggressive undermining runs the risk of damaging underlying neuro- vascular structures confined within a small space. Options become pretty limited.
For minor cases of skin avulsion, where the problem is simply the nuisance of uncontrolled bleeding, I actually recommend a simple technique using tissue adhesive glue and a tourniquet. I published a description of the technique last year, which you can read more about here.
The focus of this post is how to repair a more extensive injury. The solution I propose here is a little more labor intensive, and a little more risky: using a hypothenar skin autograft.
With the patient’s consent–and my disclosure that I couldn’t guarantee the graft would take–we proceeded. Here’s a video outlining the highlights of the procedure.
The Technique
Hypothenar skin grafts for fingertip reconstruction were first described in a modest case series in 1983 in the Journal of Hand Surgery. A portion of skin that has similar characteristics (in terms of epidermal thickness, pigmentation) to the lost skin, and comes from an area where donation will not result in any significant compromise or risk (such as unacceptable scarring or contractures limiting function) is excised, transferred, and secured with sutures. This provides epithelial coverage and gives the patient the best chance of healing with a more normal appearing finger.
The technique, in detail, is exactly as it sounds:
- First, the injury site is prepared. If there is a fingertip injury with bone projecting beyond the skin margin, it is rongeured to a level just shorter than the surrounding soft tissue.
- The defect is measured and an appropriate donor site is measured and outlined with a surgical marker. Measure carefully, this is a critical step! Per this study, a donor site as large as 2 x 6 cm can be taken.
- Excise the donor tissue as a full thickness graft, but leave behind as much fat and subcutaneous tissue as possible.
- The donor tissue is then de-fatted by inverting it and using sharp sterile scissors.
- The graft is then sutured to the donor site with simple interrupted non-absorbable sutures (silk sutures used in this study). The authors of this series recommend leaving the sutures long and tying them over a bolus dressing.
- The finger is then protected with a sterile dressing and a padded aluminum splint.
- Finally, the donor site is closed with 3-0 non-absorbable simple interrupted sutures.
- The transplant skin sutures are removed at 10 days, and the sutures at the donor site are removed at 3 weeks.
The authors of this series followed 20 patients with a total of 25 fingertip injuries treated in this fashion for an average follow up period of 9.5 months. Objective measurements were made of (1) cosmesis, (2) light touch, (3) two-point discrimination, (4) texture discrimination, and (5) dexterity using a pick-up test.
Regarding these measures:
(1) Cosmesis: The healed digits were mostly rated by patients as good, with just a few rated as acceptable, and none rated as poor.
(2) Light touch: three patients felt light touch was normal, and all but one could feel the same number of stimuli as compared to the normal fingers of the uninjured hand.
(3) Two-point discrimination: In 18 of 21 testable digits, two-point discrimination was 10 mm or less, and in 9 digits it was 6 mm or less (considered normal).
(4) All but two grafts had the ability to differentiate between very coarse and smooth surfaces.
(5) Only two digits had a 5 second or greater difference between the normal and injured hands in dexterity in picking up objects.
Case Discussion/Resolution


Performing this technique in an ED is not easy! Here’s a few of the learning points for me, based on this experience:
(1) Make sure you have time. While the video above distills the technique in to 6 minutes of highlights, actually performing the procedure, from start to finish, took me about one hour. This may not always be an option for a busy emergency physician. When I started the procedure, I had no patients waiting to be seen…when I finished, there were about six.
(2) Be prepared for bleeding. The ideal candidate for this procedure is young and healthy, and thus excision of a tissue flap will be a bloody mess. Preparing with a pneumatic tourniquet system is a smart idea. I didn’t–and I almost had a vasovagal reaction from the blood spilling on my clogs.
(3) Prep your patient for a potentially complex and prolonged healing process. As this is essentially a mini-surgical procedure, standard traumatic laceration discharge instructions won’t suffice. My patient was a casual smoker and I performed the procedure only upon his promise that he would quit, reinforcing that this could compromise the healing process. I splinted his finger (given the location over a joint) to minimize movement and allow the graft to take. Although the patient had his sutures removed in the timeline specified above, he actually wasn’t able to return to work for 6 weeks. (This mirrors the experience from the study cited above: on average, time lost from work was 39 days.)

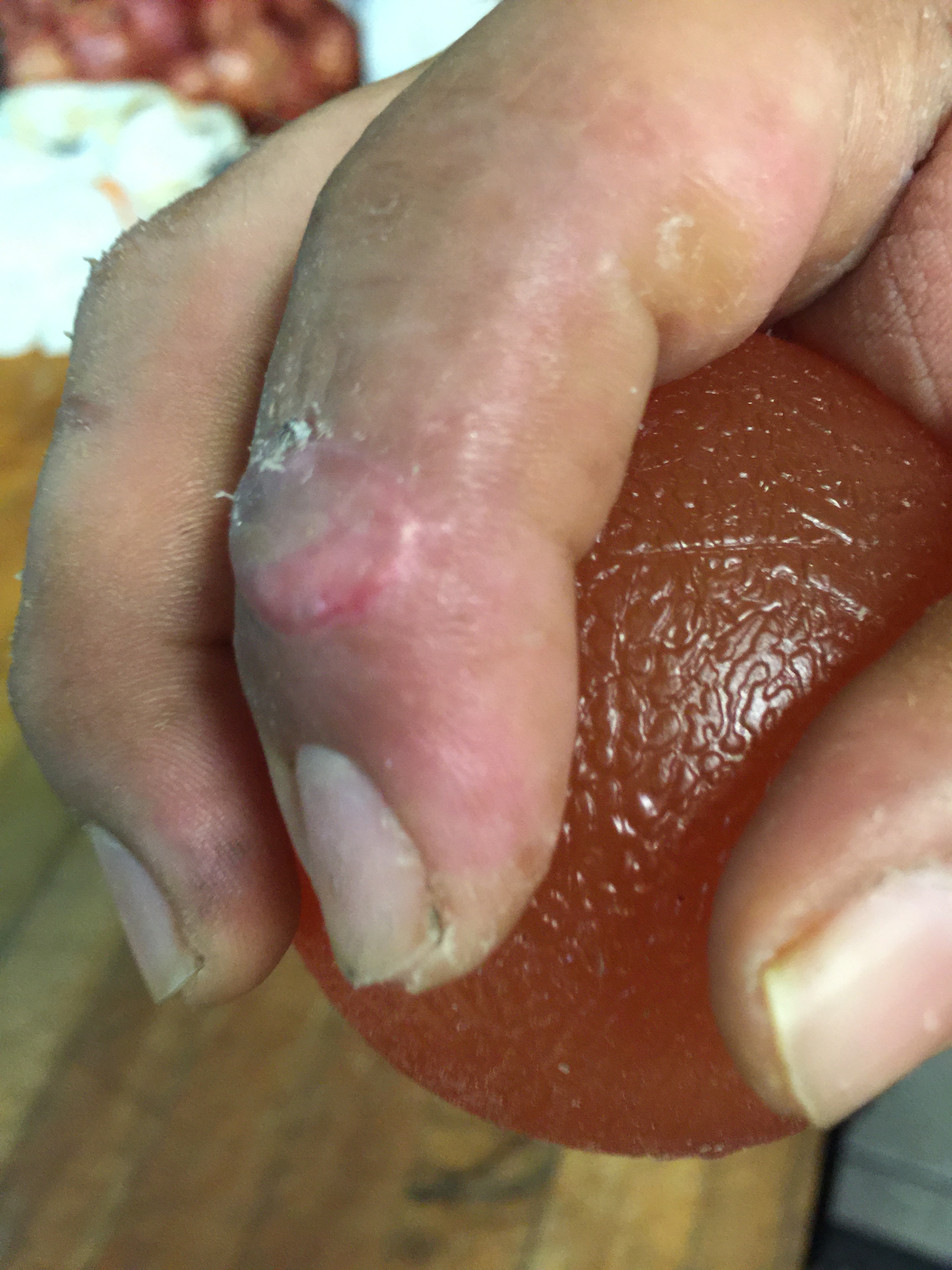
I’ve been asked by colleagues if I would undertake this procedure again in the ED. Truthfully, it took much more time and effort to perform than I anticipated. And I have to admit, I was breaking a sweat when I contacted the patient in follow up on a weekly basis, waiting to see if the graft would actually take. But when the patient finally sent me the pictures of his healed finger, he also commented: “I have no words to thank you for what you did for me.” It was a great feeling to know that took a little risk to give someone a better outcome, and succeeded. So for me, the answer is,

