In Part I of this post, I presented a clinical case where a serious arterial injury was almost missed. I also discussed some of the options for obtaining hemostasis when dealing with a small arterial “pumper.” In Part II, I’d like to focus on the technical aspects of small vessel ligation.
There may be situations where you will need to tie off a small arterial vessel to achieve hemostasis within a wound. Thus, it pays to make sure you have mastered a few “back pocket” techniques so that you are prepared to stop that bleeding…this is not the kind of skill I recommend waiting to learn until the situation actually arises!
Once again, I’ll frame the discussion with a real patient. The 80-year-old female featured in the video below fainted and hit her forehead. She sustained a short, but deep, forehead laceration. After anesthetizing, irrigating, and exploring the laceration, I discovered a troublesome little arterial bleed within the wound. I had injected lidocaine with epinephrine into the wound with little improvement. At this point I needed to definitively obtain hemostasis before I could close the wound. Watch the accompanying video to see what happened.*
*If you had trouble following the techniques used in the video above, don’t worry. I’ve reenacted the bleeding vessel ligation on a model I created for teaching purposes, which you will find below.
The situation featured in this video is one we come across relatively frequently as emergency providers. When a traumatic laceration severs even a small arteriole, the bleeding from the wound can be fairly impressive. Further complicating the issue: typically the ends of the injured vessel retract in to the margins of the surrounding damaged tissue. Thus, what you’ll see is blood pumping out from the wound without really seeing a clear source. If you are lucky and that bleeder is in the distal portion of a limb, you can tourniquet the extremity. In that case you might be able to find and clamp the vessel end to facilitate a smoother ligation. But, there will be some situations, as in this one, where that’s not really an option. You can’t really tourniquet the neck…or at least, I don’t recommend it.
And so, on to the heart of the discussion:
Here are three basic techniques for ligating a small vessel in a traumatic wound.
One. When you have clear exposure of the end of the vessel, and a second assist, it may be as simple as placing a clamp near the severed end of the vessel, then using a one- or two-handed surgical knot to ligate the end of the vessel. A short demo video on a model is shown here.
When you can’t see the end of the vessel, the options for hemostasis are a little different.
Two. The second ligation method is application of a figure-of-eight stitch around the vessel. This is not a ligation of the vessel per se, but serves to compress the surrounding tissue such that the vessel is squeezed closed and stops bleeding. In the patient video above, my attempt at a figure-of eight didn’t work–because (based upon personal review of the video after the fact) I did it wrong. Here, in the model demonstration, it’s done correctly:
Three. The final ligation method is application of a horizontal mattress suture around the vessel. The principle is the same as the figure-of-eight technique. The suture is placed around the tissue surrounding the vessel to put the squeeze on it and obtain hemostasis. This was how I ultimately stopped the bleeding in the patient we discussed. A video demonstrating the method is shown here:
The disadvantages to these two blind methods of vessel ligation is that compression of the surrounding tissue can lead to necrosis and devitalization of tissue within the wound. Thus, when possible, directly ligating the bleeding vessel is the better option. However, when it comes down to it, you need to do whatever will work in a given situation!
To close this thread, how was the outcome for the patient from the featured video?
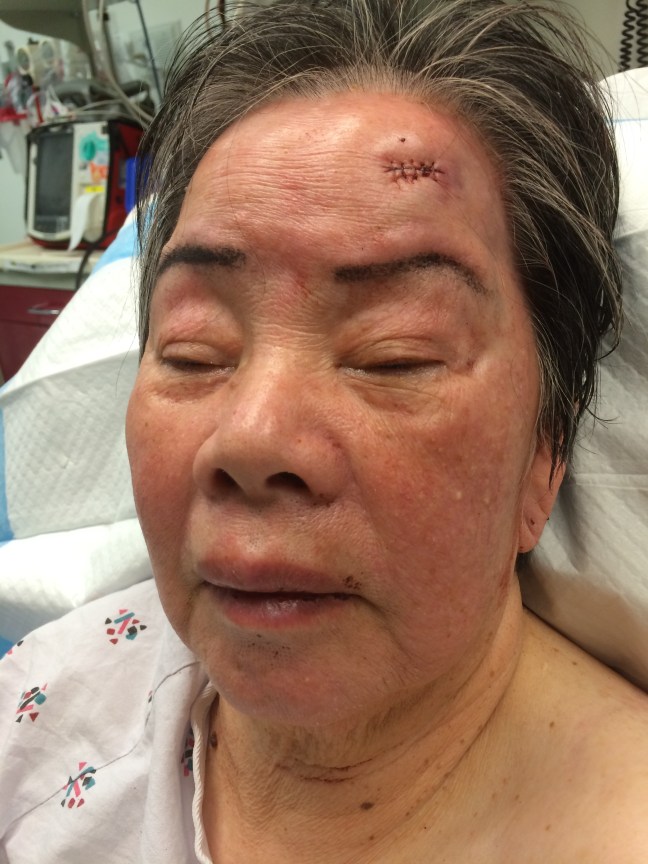 After ligation of a small arterial pumper, the wound was closed with fast absorbing plain gut absorbable sutures.
After ligation of a small arterial pumper, the wound was closed with fast absorbing plain gut absorbable sutures.Fortunately, after the bleeding was controlled the laceration itself was closed easily. The placement of the buried horizontal mattress suture also served to remove tension from the wound. The patient didn’t have great mobility and getting to a follow up visit was anticipated to be difficult, thus I chose simple interrupted fast absorbing plain gut sutures for the skin closure. Not familiar with the use of absorbable sutures for skin closure? Read here for more details.

