A 19-year-old female presented to the Urgent Care for evaluation of a facial laceration due to a bite from a friend’s dog. The patient was otherwise healthy, including an up-to-date tetanus vaccine. The dog was also fully vaccinated, including rabies vaccination series. The history was reasonable for a provoked attack by the dog due to a perceived threat.
For cosmetic reasons, both the patient and physician (me) felt primary closure was indicated.
The case raises several questions in regards to best wound care practices:
(1) How would you anesthetize & irrigate this wound?
(2) Common teaching is that mammalian bites carry a higher infection risk. What is the evidence for/against primary closure of a facial dog bite injury?
(3) How would you approach primary closure?
(4) Are prophylactic antibiotics routinely indicated for dog bite injuries?
In this two-part post, let’s first address questions (1) and (2).
(1) How would you anesthetize & irrigate this wound?
I would avoid local injection. This is an already highly contaminated wound site. Firstly, local anesthesia would further inoculate pathogenic bacteria into the surrounding soft tissue. Secondly, it would distort the margins of a wound that involves sensitive regions of the face including the vermillion border of the lip. I would opt for an infraorbital nerve block, and might even consider performing it on both sides of the face to ensure that the most medial margin of this wound (which approaches midline, where there can be some cross innervation from the contralateral side) is anesthetized.
Irrigation is a tougher question. While I generally try to avoid high pressure irrigation on (relatively) clean wounds on the face (per the results of Dr. Singer’s important 1996 Annals of EM study), it’s hard to argue with the fact that this wound is dirty and infection risk is higher. I opted for irrigation with 500 cc of normal saline via a high pressure delivery system, based on a common sense goal of balancing wound cleansing against wound edge distortion. Notably, volumes as small as 50 cc have been used to define irrigation (read on). Admittedly, this is an area not well studied.
 (Generally) peaceful stray dogs, pictured in San Pedro de Atacama, Chile, where dogs commonly run free on the street.
(Generally) peaceful stray dogs, pictured in San Pedro de Atacama, Chile, where dogs commonly run free on the street.(2) What is the evidence for/against primary closure of a facial dog bite injury?
Classic teaching is to forego attempts at primary closure of less cosmetically sensitive areas due to dog bites, such as the lower extremities. In most of these instances, marginal cosmetic benefit doesn’t really justify the increased infection risk. However, the scale is tipped with cosmetically sensitive areas such as the face. But what do we really know, and what do we tell our patients?
The first modern prospective randomized trial addressing this question was published in 1988.
Nuts & Bolts:
- Prospective, randomized trial comparing primary closure to healing by secondary intention.
- Primary outcomes: infection, cosmesis
- 96 patients with 169 total lacerations, all thoroughly debrided/irrigated. No prophylactic antibiotics. 92 sutured, 77 left open.
- Overall infection rate 7.7%. No significant difference between groups, though more infections occurred in the hands in both groups.
- Conclusion: dog bites should be thoroughly debrided, but can be safely sutured at presentation.
Some additional interesting points of discussion with regards to this study: the authors state these wounds should receive “thorough surgical treatment,” but in reality it is unclear how much debridement was performed for any given wound. Also, they define irrigation as just 50 ml delivered via a 20 ml syringe with a 19G needle.
Supportive findings were reported in a 2013 prospective randomized trial on the topic, which focused specifically on injuries involving the face.
Nuts & Bolts:
- 600 facial lacerations caused by dog bites, randomized in to a primary closure and closure-by-secondary-intention group.
- No prophylactic antibiotics given.
- Infection rates were low (8.3%, 6.3%), not statistically different between groups, and similar to those reported in previous studies.
- Interestingly, healing time was shorter in the primary closure group by just a few days [6.57 ± 0.49 days vs. 9.12 ± 1.30 days, respectively (P<0.05)].
Finally, retrospective review of cases of pediatric facial injury from dog bites treated with primary closure (2011) and adult facial injury from dog bites treated with primary closure (2014), failed to detect any association with increased infection risk with the use of primary closure. The study formats are inferior and not worth discussing in detail, but do support the use of primary closure.
Interpretation & Summary
The existing body of literature on this topic is scant, but overall suggests primary closure of facial dog bites is safe. Why is it that facial dog bites don’t get infected with increased frequency (assuming other areas of the body do)? Rationale for the results of these studies include: the relative cleanliness of the face relative to other parts of the body; the potential bias of increased attention to wound preparation in these patients; and the involvement of specialists such as plastic surgeons to perform closure.
What ever the true reason, it does seem that these wounds all warrant an attempt at primary closure on presentation, without overly worrying about additional risk conferred by the fact it’s a bite wound.
Up next:
How would you approach primary closure? And, are prophylactic antibiotics routinely indicated for dog bite injuries? To follow in Part II.


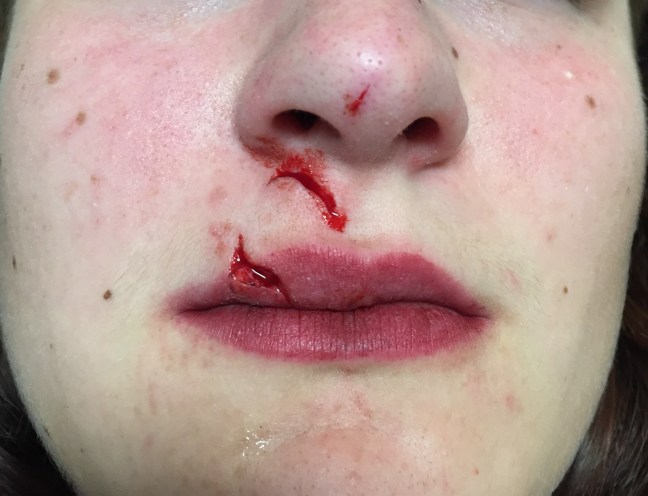 Lacerations caused by a dog bite. The upper and lower jaws of the dog are perfectly outlined in this full thickness laceration; the lower laceration is stellate and crosses the vermillion border of the upper lip.
Lacerations caused by a dog bite. The upper and lower jaws of the dog are perfectly outlined in this full thickness laceration; the lower laceration is stellate and crosses the vermillion border of the upper lip.