In the first part of this post, I discussed a case of a referral of a patient for delayed primary closure*(DPC) which was deemed inappropriate by a consulting plastic surgeon. Here in Part II, we’ll address the answer to the second question this case posed:
Question 2: What is the evidence for/against use of delayed primary closure of a traumatic laceration?
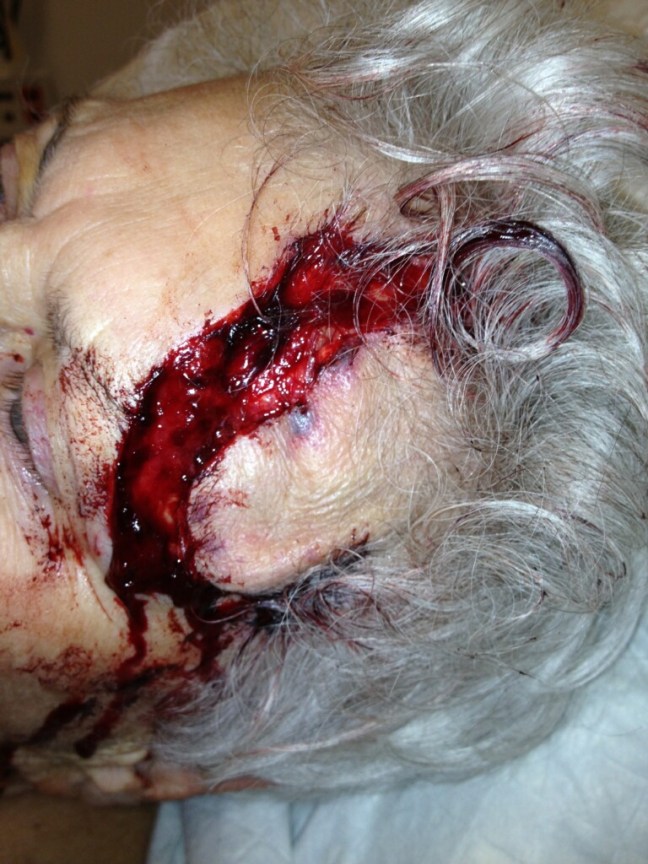
DPC: The Basic Science Perspective
Why would such a strategy even make sense? Bacterial colonization increases as a wound ages, which would lead one to believe that a wound would become more prone to infection with passage of time. This is why that wound in the case discussed in Part I was left open in the first place, right?
Half right. As a wound ages, a second simultaneous process occurs. Increased blood flow occurs at the wound edges. This improved blood flow leads to recruitment of functional phagocytes to the wound, and an increased resistance to infection. This is not just theoretical, but proven in the lab: a classic 1933 experiment in which Staph aureus was inoculated in to surgical wounds in guinea pigs at intervals demonstrated this phenomenon. At 6 hours, 100% of wounds became infected; 24 hours later, 66% became infected; 4 days after inoculation, 10% were infected; and 5-7 days after inculation, no wound became infected! Another study found that with each passing day after a wound is created, it takes a 10-fold increase in bacterial inoculation to cause infection (up to 6 days).
DPC: A Historical Perspective
To further understand the rational for DPC in clinical practice, it’s important to understand how this concept was born. DPC was a commonly used technique for traumatic injuries during World War I. At this time, antibiotics hadn’t been discovered, and so a wait-and-see-if-this-gets-infected approach was really the only option available. An interesting, in-depth discussion of war-time management of wounds and other traumatic injuries can be found here. The article elaborates on how the strategy of DPC was actually employed initially on soft tissue injuries–out of necessity rather than rigorous scientific validation.
DPC: The Evidence…or Lack Thereof
The technique was only formally studied for the first time in 1963, when the first randomized controlled trial on the subject showed a decrease from 42% to 8% incidence of infection with the use of DPC…in the operative setting. Another older study of DPC in the surgical literature boasted no infections in a series of 300 highly contaminated wounds. More recently, a 2013 meta-analysis from JAMA Surgery suggested that in contaminated or dirty abdominal wounds, DPC reduced the chances of surgical site infection. However, the authors note that the significance of this benefit was dependent on the statistical handling of the data.
This evidence seems to support DPC. However, the plastic surgeon who opposed DPC in this case may have had a valid point: DPC has never been studied for use in traumatic lacerations–ironically, the situation for which it was originally conceived. This was confirmed in a 2013 Cochrane review.
In summary: DPC was conceptualized and initially utilized for soft tissue injuries, including traumatic lacerations…but in present day it has been studied and practiced primarily in surgical clean contaminated wounds. Where does that leave us?

Bottom Line
We can wax poetical all day about the concept, the evidence, and the basic science surrounding DPC, but the reality is that DPC can’t occur unless:
- you work in a closed hospital system with a robust mechanism for ensuring proper, timely follow up of these patients;
- you associate with an urgent care or surgical clinic with skilled providers willing to perform the delayed closure;
- and you have a general consensus between your ED and follow-up providers that (despite a lack of solid evidence) this is the best management for your patients.
I don’t foresee an RCT on DPC for ED patients coming any time soon. I think it is a matter of first estimating the patient’s actual risk of primary closure and discussing this with the patient. Then, if you believe DPC is truly the best plan for your patient, ensure that the logistics of arranging a DPC in your health care system have been properly delineated.
————–
*Footnote: The case described reflects the clinical issues encountered in a real clinical encounter, to the best of my knowledge. It was referred to me by a third party. Some details of the case have been changed to protect patient identity. The discussion of the case is meant to aid medical professionals in making optimal decisions for the best care of their patients, and is not to be construed as a legal discussion. It reflects my personal opinions as shaped by the best available medical literature as of the original publication date of this blog.

