
A 19-year-old female presented to the Urgent Care for evaluation of a facial laceration due to a bite from a friend’s dog. The patient was otherwise healthy, including an up-to-date tetanus vaccine. The dog was also fully vaccinated, including rabies vaccination. The history was reasonable for a provoked attack by the dog.
For cosmetic reasons, both the patient and physician felt primary closure was indicated.
The case raises several questions in regards to best wound care practices:
(1) How would you anesthetize & irrigate this wound?
(2) What is the evidence for/against primary closure of a dog bite injury?
(3) How would you approach primary closure?
(4) Are prophylactic antibiotics routinely indicated for dog bite injuries?
In Part I, I addressed the first two questions. In this second part of a two-part post, I will now address questions (3) and (4).
(3) How would you approach primary closure?
This is undoubtedly a tricky wound. Two discrete full thickness lacerations are present. After preparing the wounds, I used almost exclusively simple interrupted 6-0 nylon sutures to close each wound. While it is a more time-consuming technique compared with placement of running sutures, in a case like this with a macerated wound in a highly cosmetic area, it’s worth the extra time to have that level of precision.
In this case I would avoid placement of deep sutures. This wound has minimal tissue loss and low tension such that deep sutures don’t add much, but they do present another nidus for infection in an already contaminated wound.
The very first suture I placed in the inferior wound was actually a corner stitch, meant to carefully approximate the edges of the “Y” shape in the center of the wound. As the laceration crosses the vermillion border, I would typically consider extra measures to ensure exact approximation at this critical junction. Fortunately, the patient’s red lipstick has already done this for me! After this, the closure follows standard technique for lip lacerations.
With regards to planar vs. everted wound closure, it’s really dealer’s choice based on a recent study from the Journal of Dermatologic surgery. While I typically strive for “the perfect suture” which is a technique focusing on eversion, in this case I believe a planar closure is best. Too much focus on everting one of the wounds might potentially pull tissue away from the second parallel wound, effectively leading to higher tension and distortion of the second wound.
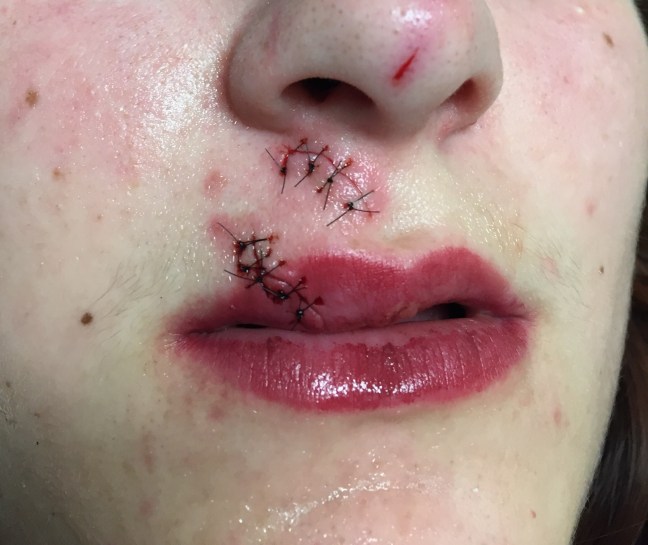
The tiny wound on the tip of the nose I simply left alone. While one might be tempted to use a tissue adhesive glue, remember this is a dirty wound and a layer of glue may theoretically seal in harmful bacteria (while I’ve not seen data on the topic, I have definitely seen infections occur with this treatment method!). Further, allowing the more superficial wound to heal by secondary intention will likely result in a great cosmetic outcome. Less is sometimes more!
(4) Are prophylactic antibiotics routinely indicated for mammalian bite injuries?
Before answering this question, let’s first deep dive in to the research that’s been done in the topic in our field.
The first relevant sub-question: What type of microbes make a mammalian bite more worrisome than your average traumatic laceration?
Many years ago, the Emergency Medicine Animal Bite Infection Study Group took cultures from over 100 patients with infected dog and cat bite wounds to see just what was growing within these wounds. They learned that infected dog and cat bites involved a complex mix of microbes different from your run-of-the-mill traumatic laceration. These included species specific to the animal’s mouth such as Pasteurella canis in dogs, as well as normal human skin flora such as Staphylococcus and Streptococcus species. I am simplifying a seminal study here for brevity, but the bottom line is that these bacteria were all generally responsive to treatment with beta-lactams with a beta-lactamase inhibitor like amoxicillin/clavulunate (trade name Augmentin, hence the oft-used term, “dog-mentin”).
So, given these yucky cooties, should we be giving antibiotic prophylaxis?
A Cochrane review on the topic was published in 2001, and reviewed anew in 2008. The meta-analysis included 8 studies (6 studies of dog bites, 1 study of cat bites, one study of human bites). Summarizing the available data at the time, the authors determined that:
- antibiotics reduce the risk of infection from human bites
- there is no evidence for use of prophylactic antibiotics for dog and cat bites
- with respect to bite location (rather than perpetrator of the bite), weak evidence supports use of antibiotics to prevent infection of hand bites
Now here’s the problems with taking these findings as gospel:
- each of the individual studies was small, so it’s difficult to rule out the possibility that a benefit of prophylactic antibiotics exists, but wasn’t detected (Type II error).
- studies were of variable quality and had significant heterogeneity.
- variable antibiotics were used in each of these studies, ranging from penicillin to co-trimoxazole to erythromycin. As we learned above from the EM Animal Bite Infection Study Group, some of these antibiotic choices may have been sub-optimal. This influences the validity of each individual study, and thus the meta-analysis as a whole.
The European Journal of Hand Surgery published a meta-analysis up-to-date as of 2012 which did not yield any game-changing findings.
This is the (lack of) evidence for routine prophylactic treatment of dog bites; and yet it seems typical in community practice to provide prophylactic antibiotics to patients with any type of bite wound injury, on any part of the body. (Comment below if you practice differently.)
Why? We know some of these wounds will get infected, and most physicians in community practice will attest to the fact that they seem to get infected more often than non-bite traumatic injuries. Maybe this is one of those processes where we’ve decided to forego scrutiny of the data to drive a decision that seems logical: if the number needed to harm is high, and that harm is generally minor (eg antibiotic side effects like diarrhea) isn’t it worth it for the benefit of preventing an infection?
Or, might we better select the patients who will actually derive benefit in these situations? Dr. Quinn and his co-investigators seem to think so. In a cost-effective analysis published in 2010, his group argued that we would be better off trying to hone in on high risk wounds rather than simply blasting all bites with antibiotics.
The results of a follow up study attempted to determine which specific dog bite injury patterns are at highest risk for infection. The findings: puncture wounds (OR of infection= 4.1 [95% CI 1.4 to 11.7]) and wounds primarily closed (OR of infection = 3.1 [95% CI 1.03 to 9.0]) were determined to be at highest risk for infection, and thus the ones most likely to benefit from prophylactic antibiotics.
Interpretation & Summary
Although the mouth of a dog (or any animal, including a human, for that matter) is proven in lab studies to be a dirty place, as it turns out most dog bite injuries probably won’t benefit from antibiotic prophylaxis. The patients most likely to benefit are those with puncture wounds or in whom primary closure is performed. The antibiotic of choice is amoxicillin/clavulunate. Given my decision to close the wound, I sent this patient out with a 5 day course of amoxicillin-clavulunate.
Her wound did not get infected on my personal follow up, and though the wound is still in the scar maturation phase, she’s pleased with the outcome thus far and gave permission for posting of these photographs:



